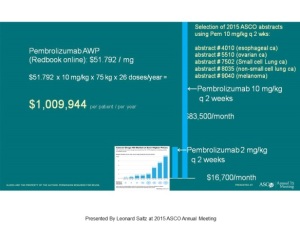
Below is the presentation I gave to the Virginia Mason Board of Directors in Seattle, Washington, on 14-July-2015.
————————————

Thank you for inviting me to speak to you today. I’ve been a patient of Virginia Mason since 1987, and am grateful for the excellent care I received and the wonderful healthcare providers I’ve come to know. Today I’m going to tell you about my journey as a metastatic lung cancer patient, and how being an engaged patient in online communities has helped keep me alive. Evidence shows being an engaged patient improves outcomes for the patient and reduces costs for the healthcare system. I’ll also share some ideas based research and my own experience that can help Virginia Mason increase patient engagement.

In early 2011, I had a nagging cough [hack hack]. To make my husband happy, I went to see my doctor. After two rounds of antibiotics, and weeks of diagnostic procedures, I was diagnosed with Stage 3a non-small cell lung cancer in May of 2011. I never smoked anything – except a salmon.

After a month’s delay to treat obstructive pneumonia, I had concurrent chemo and radiation. My primary tumor and lymph nodes all responded. Two months later, a PET scan found a new hotspot on my collarbone. A biopsy confirmed my cancer had progressed. Since I had severe lung inflammation, my oncologist recommended a break from treatment. In the next three months, I grew a 3-inch mass on my collarbone.

I had more chemo, followed by more radiation. A new scan showed all the known tumors were gone or dead. BUT … I had two new tumors in my other lung. I now had metastatic lung cancer. Whenever I stopped treatment, I had a new tumor within two months. My oncologist told me I would be on chemo for the rest of my life. Fortunately, just after I began first-line treatment, a friend and fellow cancer patient recommended I join an online support group for lung cancer patients.

In my online lung cancer community of over 20,000 people, I found patients with my type of lung cancer, on the same treatment, who understood exactly what I was feeling and experiencing. They answered questions I didn’t think to ask at doctors appointments while I was still in shock over my diagnosis. They suggested ways to cope with side effects at home. They prodded me to ask my doctor about issues I hadn’t thought were important. They were available in the wee hours when the fear was overwhelming. They shared online information resources from reliable authorities like the National Cancer Institute.
Online patient and caregiver communities form around specific diseases or treatments on patient-centered forums, social media sites, and disease advocacy organization sites. Patient blogs describe individual disease experiences and advocacy efforts on a variety of platforms and media. Some online communities connect patients and caregivers with researchers and clinicians. Patients can learn more about their diseases and treatments on trusted sites such as government agencies, medical societies, academic cancer centers, and cancer advocacy organizations. The Internet also offers information about treatment facilities and healthcare providers.

The information I learned on Inspire enabled me to become an interactive participant in my care. From other epatients, I learned to ask for my data, including radiology and pathology reports. I also learned more extensive molecular testing was available at other facilities. After my first progression, I arranged to have my slides sent to the University of Colorado Hospital for testing under the Lung Cancer Mutation Consortium Protocol clinical trial. Unfortunately, all tests were negative, but I was pleased that my Virginia Mason doctors took an interest in my test results.

I learned about clinical trials through my online patient community and searching clinicaltrials.gov. Another epatient told me I fit the profile of patients who had the ROS1 translocation—I was relatively young, had adenocarcinoma, was a never smoker, and tested negative for the three most common mutations. He told me about the ROS1 trial, which he was in, and sent me the journal article with initial results as soon as it was published. However, my Virginia Mason team had not heard of ROS1, and did not know how to test for it.

I didn’t act on the information immediately because I was already in treatment. However, after my second progression, I contacted University of Colorado again, and learned they had recently developed a ROS1 test. I gave them permission to test my remaining slides. When I learned my cancer was ROS1 positive, my Virginia Mason team was enthusiastic and worked quickly to determine whether my new lung nodules were cancer. When one of the nodules grew 50% in one month, they agreed I should try the ROS1 crizotinib trial, and I enrolled at University of Colorado in November 2012.

Thanks to precision medicine and the online lung cancer community, I’ve had No Evidence of Disease for 30 months. I’m not cured, but life is relatively normal for now–if you ignore the scanxiety every 8 weeks. I will eventually develop resistance to this drug, but I know other clinical trial options are now open to me.

I am alive because I am an e-patient. E-Patients are not just patients who go online to find information. The are any patient who is equipped, engaged, empowered, and enabled. Because I became an e-patient, I was able to actively participate as a partner in shared decision making with my healthcare providers. I was able to express my goals for my care, and my Virginia Mason providers incorporated my values into our discussions.
When my oncologist suggested I take Alimta chemo for my second line treatment, I suggested that we consider adding Avastin. Even though that was a more aggressive treatment, my oncologist agreed because he knew I understood the risks as well as the potential benefits. My Virginia Mason doctors did not suggest shared decision making or offer me any decision aids, but they were very open to discussing options with me when I initiated the conversation.

Preliminary studies indicate patient engagement and shared decision making can increase patient satisfaction and outcomes and reduce healthcare costs. Activated patients are less likely to be readmitted within 30 days of discharge, less likely to have poor care coordination across healthcare providers, and less likely to lose confidence in their health care system.
But not all patients are naturally inclined to become engaged participants in their healthcare. How can we encourage patient activation and engagement? What motivates a patient to become engaged?

The Internet is now accessible to large portion of the US population. As you might expect, the percentage is higher among younger age groups, approaching 100%, but the rate of new users is growing fastest among the Medicare crowd.

Patients are already accessing health information on mobile devices such as smartphones. Caregivers, patients facing medical crises, and patients dealing with significant health changes are more likely to use their smartphone to look for health or medical information online.

Connected health fills needs not met by the traditional healthcare system. As of 2010, the majority of Internet users have looked online for information about specific diseases or medical problems, or checked out medical treatments or procedures. And those numbers have grown over the past 5 years.
A 2013 Pew Research study of people who have access to the Internet found those living with a chronic condition are more likely to:
- Gather information online about medical problems, treatments, and drugs.
- Consult online reviews about drugs and other treatments.
- Read or watch something online about someone else’s personal health experience
- Fact check what they find online with a medical professional.
ePatients are more savvy than you may think. You might be concerned that receiving medical advice from others online is dangerous. So far, it’s not. Pew Research found 60% of Internet users who go online for health information say they’ve been helped. Only 3% say they or someone they know have been harmed.

The Internet and other connected health resources do not replace the need for healthcare providers. Research shows patients still consider their healthcare providers the most trustworthy source of health information. Rather, connected health resources save time and reduce costs by answering questions that arise after the patients have left their providers’ office or facility, providing patients with reliable information they can bring to shared decision making discussions, and encouraging patient engagement in their own care.
When I developed a hard nodule at the base of my neck after my first line treatment, it was my online support group that encouraged me to tell my provider about it sooner rather than later.

A Health Affairs Health Policy Brief, defines “patient activation” as a patient’s knowledge, skills, ability, and willingness to manage his or her own health and care. “Patient engagement” is a broader concept that combines patient activation with interventions designed to increase activation and promote positive patient behavior, such as obtaining preventive care or exercising regularly. It is these interventions, along with access to trusted information sites, that Virginia Mason can provide to its patients to promote patient engagement.

Connected health can provide tools to support care coordination. Seventy percent or more of caregivers are interested in using technologies for tracking personal health records, coordinating caregiving, and helping with medication management. Pew research studies show that 84% of women and 75% of men conduct health research online for someone else.
Connected health tools can also help patients navigate the healthcare system. Trained navigators, patient advocate translators, social media curators, adaptive search tools and shared rating systems could help patients find the most appropriate information from the most relevant trusted resource. Apps could provide information for specific diseases and treatments. Interoperative platforms could enable care coordination across silos of care, care locations, and care providers.

Virginia Mason needs to develop a patient engagement strategy to guide its efforts and meet the strategic goal within Innovation of Service for full partnerships with patients and familes. You might want to use the Healthcare Information and Management Systems Society (HIMMS) patient engagement framework as a guideline. I understand it was emailed to you before the meeting. It’s divided into five sections. I’ll use my experience as examples of what might be included in each section:
- Inform Me
- Provide my care plan and a summary of my providers on my patient portal site
- Engage Me
- Give me an app that describes my chemo’s side effects and ways to treat them
- Send my treatment schedule appointments to my smartphone and email reminders for follow-ups
- Empower Me
- Allow me to take care experience surveys online
- Transmit my medical records electronically for a second opinion [explain file cabinet example]
- Partner With Me
- Provide a care coordination platform that enables family members to select and share care duties, like transportation or meal preparation
- Provide electronic survivorship plan with schedule for follow-up and therapies
- Support My e-Community
- Offer a wearable that provides med reminders tailored to my prescriptions [example: silent alarm on my fitbit]
- Provide decision aides to help me evaluate treatment options [example: aggressive biopsy]

Providing patient engagement tools and supports can benefit the Virginia Mason system and facilities as well as patients. They can help retain patients, attract new patients, improve health outcomes, increase employee retention, attract more qualified employees, and bolster your reputation.

I hope I’ve shown you the benefits of patient engagement, and encouraged you to develop patient engagement strategies for Virginia Mason. Thank you for inviting me to share my story and perspective.